How can we make medication management, a crucial component to aging well, easier for older adults? Adhering to medication is a difficult task for older adults and few products are clinically shown to effectively improve adherence. Furthermore, it is estimated that 50% or more of U.S. adults do not take their prescriptions as directed, and that medication non-adherence is responsible for as many as 33%-69% of hospital admissions and 125,000 deaths annually.
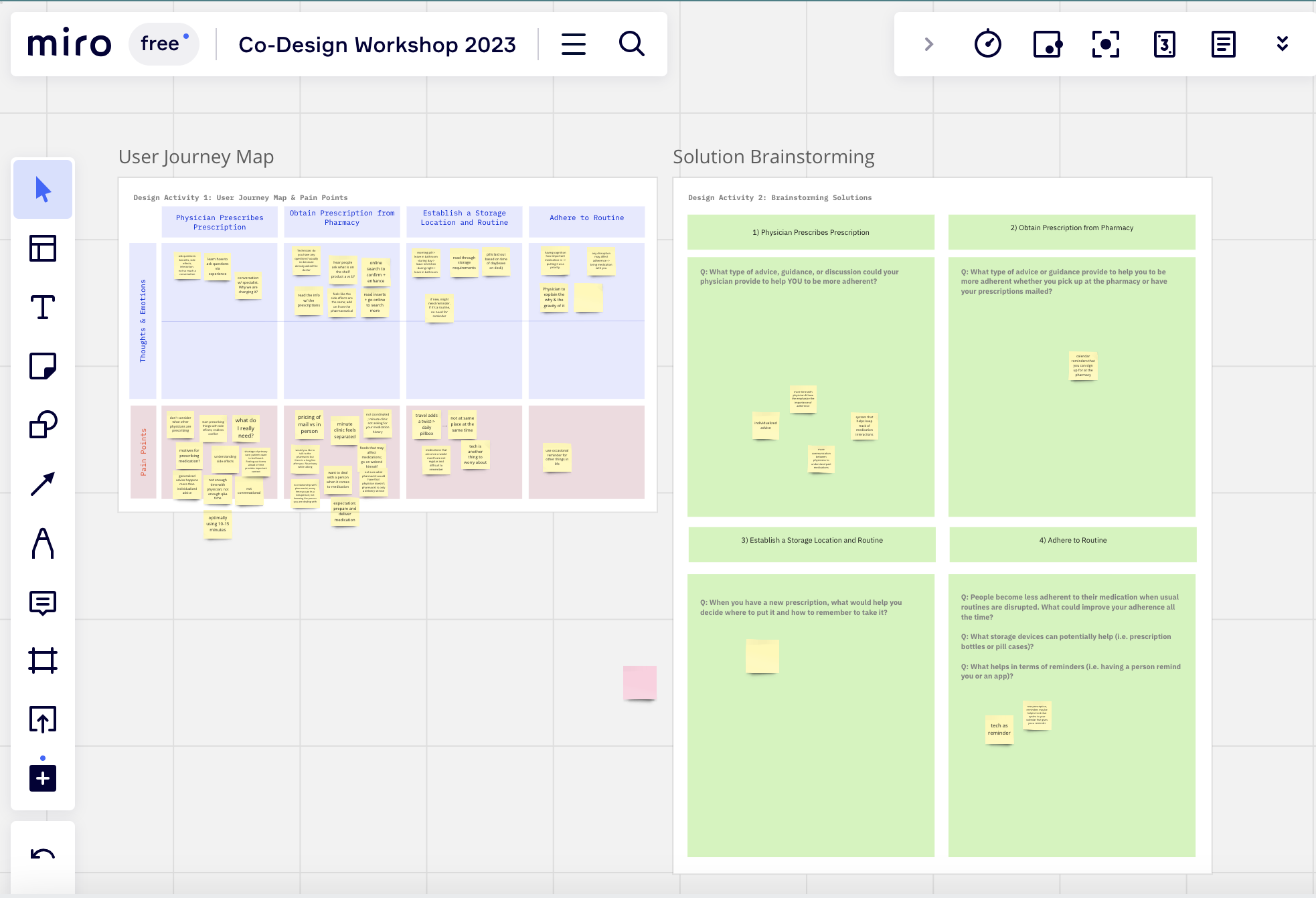
As researchers, we are interested in understanding the barriers older adults face when trying to take prescriptions as prescribed and what solutions can improve at-home medication adherence. After conducting a survey and interview study to understand adherence routines, we wanted to directly hear from older adults about what would help them develop successful adherence routines. However, current medication adherence solutions are generally designed for, instead of with, intended patient populations.
How can we make medication management, a crucial component to aging well, easier for older adults? Adhering to medication is a difficult task for older adults and few products are clinically shown to effectively improve adherence. Furthermore, it is estimated that 50% or more of U.S. adults do not take their prescriptions as directed, and that medication non-adherence is responsible for as many as 33%-69% of hospital admissions and 125,000 deaths annually.
As researchers, we are interested in understanding the barriers older adults face when trying to take prescriptions as prescribed and what solutions can improve at-home medication adherence. After conducting a survey and interview study to understand adherence routines, we wanted to directly hear from older adults about what would help them develop successful adherence routines. However, current medication adherence solutions are generally designed for, instead of with, intended patient populations.




.png)

"I came up with a scheme, where I keep the medicines on one side of my microwave, or my toaster oven. When I take it, I put it on the other side."
– Participant 4
.png)
"If I have to go somewhere, first thing in the morning, that's a typical time when I forget. Because sometimes I don't even have time for breakfast or for one reason or another didn't get around to it. Then the next day, it's Monday, but I'm looking at the Sunday case saying, ‘Oh, I guess I forgot to take it yesterday.’ " –Participant 7




People have a desire to build stronger relationships with their physicians and would be more susceptible to advice if they feel the advice giver knew them well. They want more time with their physicians to have questions fully answered and desire more personalized guidance about taking a new medication.
Since all participants did not struggle with adherence, they strongly felt that adherence was a personal responsibility and that more advice from physicians, pharmacists, or assistance from technology would not be helpful to them currently. Thus, participants had some difficulty in brainstorming solutions. Catering to this demographic, a better framing to pivot to for the workshop would have been “How can you use your experiences and success with adherence to design for others?” We can improve the workshop’s structure by presenting a “design brief,” providing more context about why people struggle with adherence.
We want to revise our recruitment strategy to target people who struggle with adherence. While discussing design solutions with individuals who are adherent gives us a special viewpoint from those who already know what makes a successful medication management strategy, they lacked perspective about why others were not adherent. By directly involving people who struggle with adherence, we can gain valuable insight into this perspective.
Following the spirit of co-design, there is huge potential in physically going to the communities we are designing for and bringing our workshop to them. We are currently planning an in person workshop with Brookhaven, a senior living community in Lexington, MA. Other future workshop locations would be nursing homes, senior centers, and assisted living facilities.
People have a desire to build stronger relationships with their physicians and would be more susceptible to advice if they feel the advice giver knew them well. They want more time with their physicians to have questions fully answered and desire more personalized guidance about taking a new medication.
Since all participants did not struggle with adherence, they strongly felt that adherence was a personal responsibility and that more advice from physicians, pharmacists, or assistance from technology would not be helpful to them currently. Thus, participants had some difficulty in brainstorming solutions. Catering to this demographic, a better framing to pivot to for the workshop would have been “How can you use your experiences and success with adherence to design for others?” We can improve the workshop’s structure by presenting a “design brief,” providing more context about why people struggle with adherence.
We want to revise our recruitment strategy to target people who struggle with adherence. While discussing design solutions with individuals who are adherent gives us a special viewpoint from those who already know what makes a successful medication management strategy, they lacked perspective about why others were not adherent. By directly involving people who struggle with adherence, we can gain valuable insight into this perspective.
Following the spirit of co-design, there is huge potential in physically going to the communities we are designing for and bringing our workshop to them. We are currently planning an in person workshop with Brookhaven, a senior living community in Lexington, MA. Other future workshop locations would be nursing homes, senior centers, and assisted living facilities.